AI Employees for Healthcare
- Administrative layer automation: An AI employee for healthcare handles scheduling, intake, insurance verification, billing and claims, follow-up communications, and compliance documentation without involvement in clinical decisions.
- Scheduling and access: AI employees manage appointment scheduling across provider availability, patient preferences, and appointment type requirements without a staff member handling each interaction individually.
- Patient intake: AI employees automate intake form collection and data population so patient records are complete and accurate before the appointment begins.
- Insurance verification: AI employees verify coverage against current payer data, flag discrepancies, and surface authorization requirements before the appointment rather than discovering issues after the fact.
- Claims accuracy: AI employees review claims for coding accuracy and payer-specific requirements before submission, reducing the denial rates that require time-consuming appeals to correct.
- Patient communications: AI employees run appointment reminders, care gap notifications, and post-visit check-ins reliably so patients receive the right information at the right time.
- Compliance monitoring: AI employees monitor regulatory updates and flag documentation gaps so organizations can address issues proactively rather than during audits.
- Top clients: We help Fortune 500, large, mid-size and startup companies with AI development, consulting, and hands-on training services. Our clients include Microsoft, Google, Broadcom, Thomson Reuters, Bank of America, Macquarie, Dell and more.
The Administrative Burden Clinic Staff Were Never Supposed to Carry
Healthcare organizations run two parallel operations: the clinical work of patient care, and the administrative work of managing access, documentation, billing, and compliance. These two operations compete for the same staff time. When a physician spends time on documentation that an administrative workflow should handle, that is time not spent with a patient. When a front desk coordinator spends an afternoon resolving a billing dispute that a better claims review process would have prevented, that is capacity not available for scheduling. The administrative burden in healthcare has grown ahead of the staffing available to absorb it: prior authorization requirements have expanded across major payers, coding complexity has increased, and compliance documentation requirements have multiplied under regulatory frameworks that update frequently. The consequences of administrative errors are not confined to the administrative function: a scheduling gap means a patient did not receive timely care, an intake error means the clinician is working from an incomplete record, and a claims error means revenue that was earned is not collected.
Insurance verification creates some of the most preventable downstream problems. When coverage has not been verified against current payer data before a patient arrives, every available option creates friction: delay the appointment, provide care and absorb billing uncertainty, or generate a difficult patient interaction. Claims denial management is where the revenue cycle impact concentrates: denials from coding errors, missing prior authorization documentation, or payer-specific submission requirements generate appeals work that is time-consuming and entirely preventable with better pre-submission review. AI employees address the administrative layer specifically, handling scheduling, intake, insurance verification, claims review, follow-up communications, and compliance monitoring, without involvement in clinical diagnosis or treatment decisions. Cazton builds AI employees in this sector with HIPAA requirements and your organization’s data handling standards as foundational design constraints, enforced through our AI governance practice.
Core Capabilities for a Healthcare Administration AI Employee
Healthcare administration AI employees cover the workflows that connect patients to care and that connect care delivery to accurate documentation and payment. The capabilities that produce the most value are those that reduce the error rates and manual handling time that drive administrative cost and revenue leakage.
Core capabilities include:
- Appointment scheduling and access management: Handle scheduling across provider availability, appointment type requirements, and patient preferences, including new patient intake, follow-up visits, and specialty referral coordination.
- Patient intake automation: Collect and validate intake forms digitally, populate EHR fields from submitted data, and flag incomplete or inconsistent information before the appointment so staff are not resolving data problems at the point of care.
- Insurance verification: Verify patient coverage against current payer data, confirm benefit details, flag authorization requirements, and surface coverage issues before the visit so they can be addressed in advance.
- Claims review and submission support: Review claims against payer-specific coding requirements, identify issues before submission, and flag denials with the relevant denial reason so the appeals process is organized rather than reactive.
- Patient communication: Send appointment reminders, follow-up care instructions, satisfaction surveys, and care gap notifications through the patient's preferred channel on defined schedules.
- Compliance monitoring: Track documentation requirements, flag records that are incomplete for audit purposes, and monitor regulatory updates that affect administrative processes or reporting obligations.
Scheduling, Intake, and Access Coordination
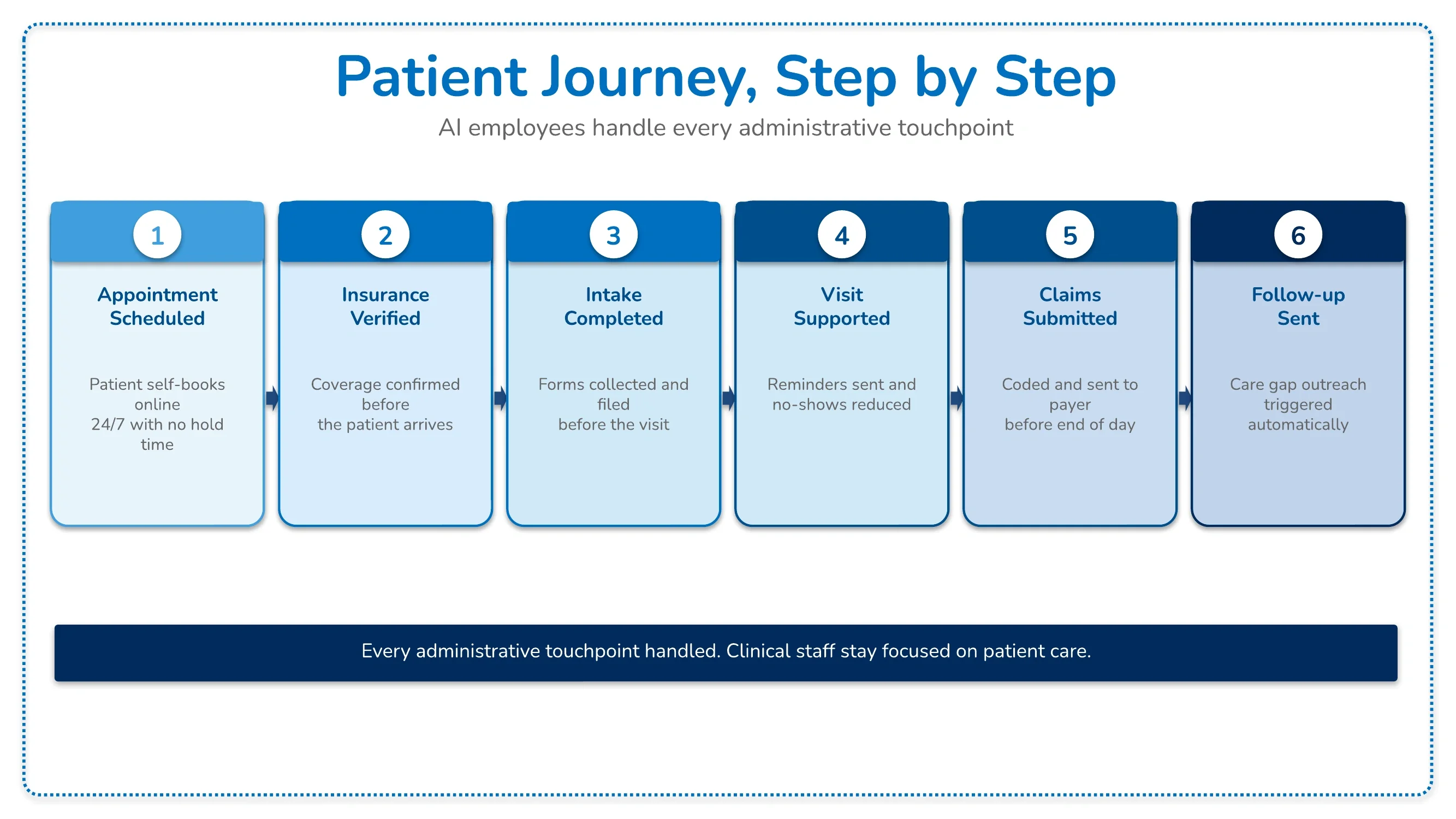
Patient access is the first administrative function that shapes the patient experience, and it is one of the most labor-intensive when handled manually. Scheduling a new patient requires coordinating appointment type requirements, provider availability, insurance verification timing, and intake form completion in a sequence that often involves multiple staff touchpoints and patient-facing back-and-forth.
AI employees handle scheduling coordination as a continuous process rather than a series of individual staff interactions. New patient scheduling initiates intake form collection automatically. Insurance verification runs in parallel with scheduling rather than requiring a separate workflow step. Appointment confirmations and reminders go out on schedule without requiring staff intervention for each patient.
The effect on front desk staff is a shift away from scheduling logistics and toward patient interactions that benefit from human attention: answering nuanced questions, handling patients who need accommodation, and managing complex situations that the AI employee is designed to escalate rather than attempt to resolve alone.
Insurance Verification and Claims Processing
Insurance verification is the administrative task most directly connected to revenue integrity, and it is one where errors or delays at the front end cascade into billing complications at the back end. A patient seen without current verification of their coverage creates a billing scenario that is harder to resolve cleanly after the fact than it would have been to identify before the visit.
AI employees run verification against current payer data before each appointment, surface any coverage changes since the patient's last visit, and flag authorization requirements for procedures or specialist visits that require pre-authorization. The information reaches the care coordination team in advance rather than surfacing at check-in.
Claims processing follows a similar pattern. An AI employee that reviews claims before submission against payer-specific requirements identifies coding issues and documentation gaps while correction is straightforward rather than after a denial requires an appeals process. Cazton's AI governance practice designs the oversight frameworks that ensure AI employees in revenue cycle functions operate within defined accuracy standards and escalate decisions that carry meaningful financial risk to human review.
Compliance, Documentation, and Data Privacy
Healthcare AI deployments operate in a regulatory environment that includes HIPAA requirements for data handling and patient privacy, documentation standards for billing and coding accuracy, and a regulatory landscape that continues to evolve. An AI employee deployed in healthcare administration needs to be built to operate within those constraints as a baseline, not retrofitted to comply with them after the fact.
Cazton builds healthcare AI employees with HIPAA-compliant data handling, access controls, and audit logging as requirements of the system architecture rather than features added after initial deployment. Patient data is handled according to the minimum necessary standard, and every access event is logged in a format that supports audit review.
Compliance monitoring adds a proactive layer. As documentation requirements evolve and payer-specific coding rules change, your AI employee surfaces the updates that affect your administrative processes so your team can adjust before the next audit or billing cycle rather than discovering gaps reactively. Cazton's AI consulting practice works with your compliance team to define the monitoring scope and alert logic that reflects your organization's specific obligations.
Healthcare System Integrations
Healthcare AI employee deployments depend on integration quality more than most industries because the consequences of data staleness are direct: an insurance verification that works from a payer lookup hours old can produce the same outcome as no verification at all on a plan that changed. A claims review that cannot access the most current payer-specific requirements flags the wrong issues. Cazton builds these integrations to EHR, payer, and billing platform APIs rather than surface-level data exports, and designs them with HIPAA security and access controls as requirements from the start. Common integration points include:
- Electronic health record platforms: Epic and Oracle Health for patient record access, scheduling data, intake information, and documentation that ties administrative workflows to the clinical record.
- Practice management systems: Athenahealth and similar platforms that manage scheduling, billing, claims, and patient communication in ambulatory care environments.
- Payer portals: Insurance verification and prior authorization APIs that allow the AI employee to verify coverage and authorization status in real time rather than through manual portal navigation.
- Patient communication platforms: Secure messaging and patient portal systems for appointment reminders, follow-up communications, and satisfaction surveys that maintain appropriate channel security for healthcare communications.
Case Studies: Healthcare Administration
When a Multi-Location Medical Group Could Not Keep Scheduling Staff Ahead of Demand
Challenge: A multi-location medical group came to Cazton with a patient access problem that was creating measurable business consequences. Their scheduling team was handling high volumes of inbound calls and online appointment requests manually, which created variable wait times, inconsistent intake form completion rates, and insurance verification gaps that were not discovered until the day of service. New patient conversion was suffering because the gap between initial inquiry and confirmed appointment was long enough that patients were scheduling with competitors.
Result: Cazton deployed an AI employee integrated with their EHR scheduling module and their payer verification connections. New patient scheduling requests initiated an automated sequence: intake form collection, insurance verification against current payer data, and appointment confirmation, without requiring a staff member to manage each step. Their scheduling coordinators shifted their time to cases that required judgment: complex scheduling needs, patients with coverage complications, and coordination for specialty referrals. The front desk team reached patients prepared for their visits rather than discovering coverage and intake gaps on arrival.
Reducing Claim Denials That Were the Result of Preventable Submission Errors
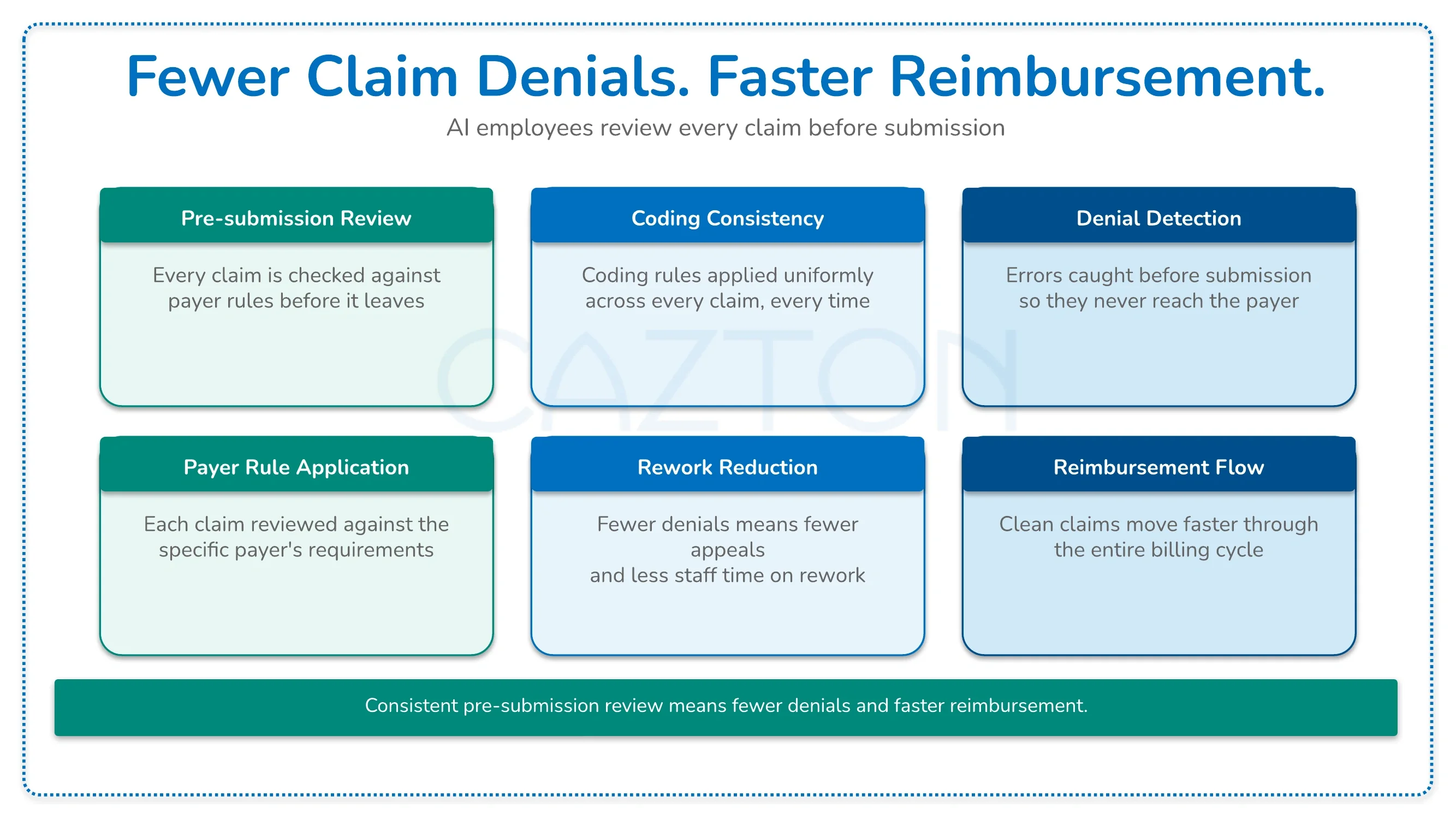
Challenge: A hospital system’s billing team was managing a claim denial volume that was consuming a disproportionate share of their revenue cycle staff capacity. Analysis of their denial patterns showed that a significant portion were arising from preventable causes: coding errors, missing prior authorization documentation, and payer-specific submission format requirements that were not consistently applied. The team was spending their time on appeals rather than on the pre-submission review that would have prevented the denials in the first place.
Result: Cazton built an AI employee that reviewed claims prior to submission, checking against payer-specific coding requirements, confirming that authorization documentation was attached where required, and flagging claims with characteristics that correlated with denial risk based on the organization’s historical denial data. The revenue cycle team received a pre-submission review report rather than a post-denial appeals queue. Their billing staff spent time on the complex claims and the cases requiring clinical documentation support, and the overall denial rate declined as preventable submission errors were caught before they created appeals work.
Giving Clinical Staff Back the Time Spent on Routine Administrative Follow-Up
Challenge: A specialty practice with a high-volume patient panel had a follow-up communications problem. Care gap notifications, post-visit instructions, referral tracking follow-up, and appointment reminders were being sent inconsistently because the staff time required to execute them was competing with the scheduling and clinical support work that occupied the same people. Patients were falling through administrative gaps that the practice knew existed but did not have the capacity to close.
Result: Cazton deployed a patient communications AI employee that integrated with their EHR and their patient messaging platform. Post-visit instructions went out automatically on the schedule their clinical team defined. Care gap notifications triggered on the conditions defined in their care management protocols. Appointment reminders and confirmation requests ran without requiring staff to initiate each communication. The clinical staff retained full control over the content and parameters of every communication type, with the AI employee executing the distribution reliably and tracking patient responses for the cases that required a human follow-up.
Building Your Healthcare Administration AI Employee with Cazton
Healthcare AI deployments require that compliance, data privacy, and the appropriate scope of AI decision-making be built into the system architecture from the beginning, not addressed after the functional capabilities are built. Cazton’s practice in healthcare administration starts with HIPAA requirements, your organization’s specific data governance standards, and the clear boundary between administrative AI and clinical decision-making. Our AI governance capabilities ensure the AI employee is designed with the controls, audit trails, and escalation paths the regulatory environment requires.
The AI employees Cazton deploys in healthcare administration handle the administrative functions precisely as designed. Clinical decision support, diagnostic assistance, and treatment recommendations are outside their scope. The value is in removing administrative burden from clinical and administrative staff so they can spend their time on the work that requires them, with an AI employee handling the scheduling, verification, communications, and documentation work that currently consumes time that should not be allocated there.
Check out more of our AI employees for your business and explore how intelligent workers are transforming operations across every major business function.
Contact Cazton to discuss an AI employee for your healthcare administration environment, whether the priority is patient access, revenue cycle integrity, or administrative compliance monitoring.
Cazton is composed of technical professionals with expertise gained all over the world and in all fields of the tech industry and we put this expertise to work for you. We serve all industries, including banking, finance, legal services, life sciences & healthcare, technology, media, and the public sector. Check out some of our services:
- Artificial Intelligence
- Big Data
- Web Development
- Mobile Development
- Desktop Development
- API Development
- Database Development
- Cloud
- DevOps
- Enterprise Search
- Blockchain
- Enterprise Architecture
Cazton has expanded into a global company, servicing clients not only across the United States, but in Oslo, Norway; Stockholm, Sweden; London, England; Berlin, Germany; Frankfurt, Germany; Paris, France; Amsterdam, Netherlands; Brussels, Belgium; Rome, Italy; Sydney, Melbourne, Australia; Quebec City, Toronto Vancouver, Montreal, Ottawa, Calgary, Edmonton, Victoria, and Winnipeg as well. In the United States, we provide our consulting and training services across various cities like Austin, Dallas, Houston, New York, New Jersey, Irvine, Los Angeles, Denver, Boulder, Charlotte, Atlanta, Orlando, Miami, San Antonio, San Diego, San Francisco, San Jose, Stamford and others. Contact us today to learn more about what our experts can do for you.


